Seasonal influenza, commonly called the flu, affects about 21 million people in the U.S.every year,1 resulting in significant burdens to the economy and public health.2 Vaccination remains the most effective way to reduce the risk of death or hospitalization, but the rate of vaccination consistently falls short of the goal of 70% set by national immunization guidelines for the U.S.3
People with diabetes face particularly high risks of complications from influenza, including impact on glycemia, pneumonia, cardiovascular events, hospitalizations, and premature death.4-6 However, although the rate of vaccination for influenza is higher in individuals living with diabetes than in the general adult population, it is still below the recommended rate of 70%. Effective and scalable solutions are needed to increase flu vaccination rates in this group across all age categories.
“Influenza vaccination is critical for persons with diabetes. In fact, a recent research study published in Diabetes Care (September 2021) underscores this importance. The study showed that influenza vaccination led to a reduced risk of approximately 15% of all-cause death, cardiovascular death, death from acute myocardial infarction or stroke, and a reduced risk of being admitted to hospital with acute complications associated with diabetes (diabetic keto acidosis, hypoglycemia, or coma),” said Neil Skolnik, Professor of Family and Community Medicine, Sidney Kimmel Medical College, Thomas JeffersonUniversity; Associate Director, Family Medicine Residency Program, AbingtonJefferson Health, and co-author of the study. “Ensuring adequate influenza vaccination is of critical importance for people with diabetes,” Skolnik added.
Digital interventions—such as general messaging, education, and incentives delivered via cellphone apps—have been effective in prospective studies of general NorthAmerican populations.7-9 In fact, the use of any healthcare information technology has been positively associated with influenza vaccine use.10 Digital interventions also might be effective in addressing other barriers to vaccination with individuals living with diabetes, such as fear of adverse reactions, belief that they are not at high risk, or misinformation about the influenza vaccine (e.g., it is ineffective, it transmits the flu, etc.).11
We analyzed the effect of six monthly digital interventions on self-reported influenza vaccine rates among 5158 U.S. adults with Type 1 or 2 diabetes and 5271 control participants in a decentralized, blinded randomized trial. The interventions were delivered through Evidation’s mobile app, an established health activity and research platform.
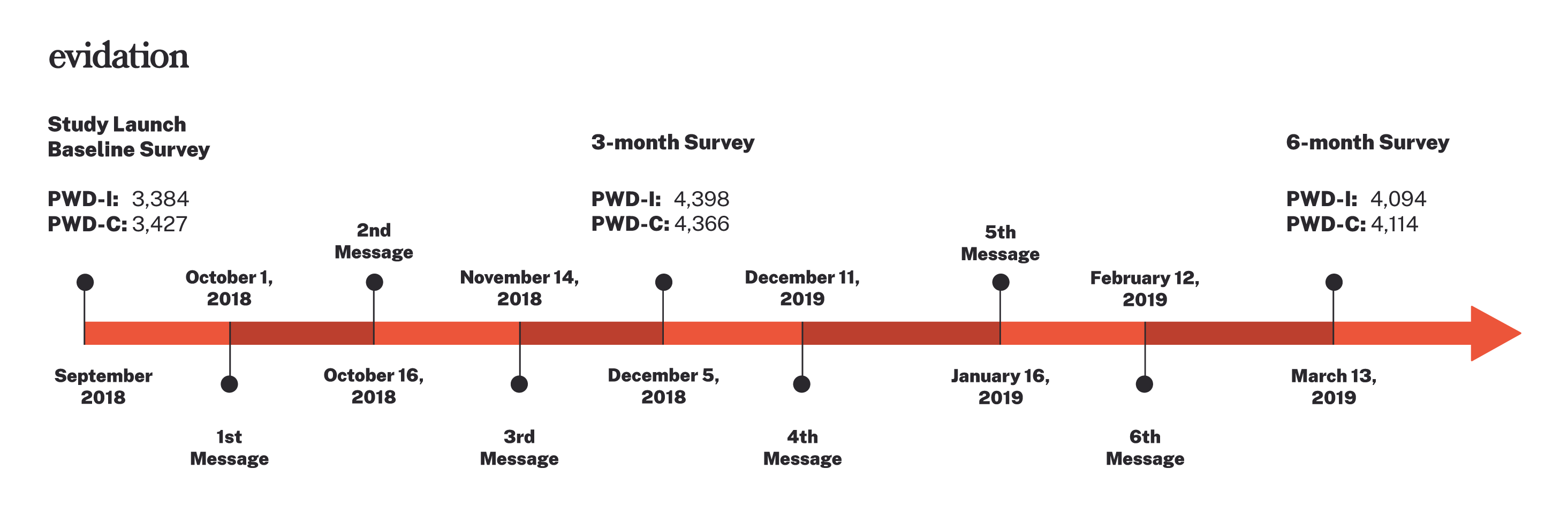
Study participants were sent offers to receive “points” as compensation for completing surveys and study tasks, a routine component of participating in the Evidation platform. An individual was compensated a maximum of $USD 0.30 for completing all interventions, thus financial motivation for vaccination was unlikely. Participants were blinded not only to their treatment assignment but also to the fact that they were enrolled in a study, a factor unique to a web-based pragmatic trial.
Each of the six monthly messages was structured in two parts: educational content, and a call to action for the participant to complete. The education and recommendations provided in the intervention reflected the then-current standard of care for people with diabetes.

The participants were predominantly white, female, middle-aged, and had high levels of income and education, representing this specific digitally-connected population. The intervention and control groups did not differ significantly on these demographic factors.
“Unique to this study was the ability to reach such a large group of at-risk individuals with minimal interference in their everyday lives, demonstrating the impact of utilizing digitally connected communities to meaningfully impact vaccination behavior in this pragmatic clinical trial,” stated Jennifer L. Lee,Behavioral Scientist at Evidation Health.
At six months, 64.2% of participants in the intervention group reported flu vaccination, compared to only 61.1% of people in the control group, for an absolute increase of 3.1% with intervention (relative improvement, 5%).Completion of at least one intervention message was associated with an absolute5.5% increase in vaccination rate (p<0.001), or a relative improvement of9%.
After adjusting for age, sex, race, and concomitant medical conditions, the intervention group remained significantly more likely to report flu vaccination than the control group (risk ratio 1.05, 95% confidence interval 1.02, 1.08,p<0.001) .
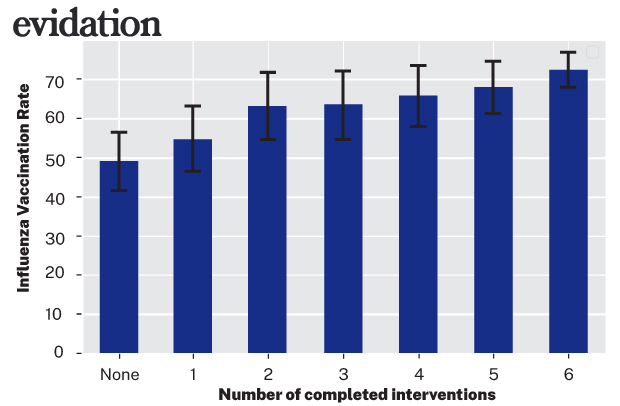
Engagement rates with interventions were high overall, with completion rates between 17%and 25% across the different messages, consistent with digital communication industry standards.12 Moreover, the vaccination rate increased as engagement increased.
Of note, participants were most likely to respond to the first two messages, with an overall decline in response rates in later months. These two messages targeted information on “The Flu and Diabetes” (October) and centered around“World Diabetes Day” (November), suggesting a possible synergy between relevant disease-focused events and intervention deployments.

Advice given by a healthcare provider to vaccinate was strongly associated with immunization in both the intervention and control groups (odds ratio 12.3; 95%confidence interval 10.2,15). This is consistent with previous work showing the importance of healthcare providers in promoting vaccination.11
Although the 3% absolute increase in vaccination rate seen in our study is much higher than that seen in other studies of digital interventions for this purpose, it was smaller than that seen in a prospective interventional study that provided compensation for vaccination (a 5% increase).7 Financial incentives might further bolster vaccination rates.
Vaccination rates did not differ significantly between groups during the first two months of messaging, but the rates diverged during later months. This might highlight the importance of repeated messaging throughout the influenza season.Alternatively, the content of the later messages themselves might have been more impactful. Additional research should clarify the impact of the timing and content of interventional messaging.
Given the total population of people with diabetes in the U.S., the absolute increase of 3.1% in flu vaccination rate could represent about 830,000 additional persons receiving the vaccine. This would substantially reduce the clinical and economic costs of the illness for both individuals and healthcare systems.
DavidKerr MD, Director of Innovation at Sansum Diabetes Research Institute and co-author of the paper emphasized, “Influenza can be dangerous for people with diabetes and an annual flu vaccine is a ‘must-have’ component of self-care.This new study shows how effective digital technology can be in making sure that as many people with diabetes as possible have their flu shot and at a very low cost. This could be a model for other vaccination programs.”
A unique strength of this web-based randomized trial was the ability to blind participants not only to their treatment assignment but also to participation itself, providing an opportunity to test how people would respond to the intervention in real-world settings. The online platform also allowed rapid enrollment with high geographic diversity, unlike most clinical trials.
The study population likely does not represent the overall US population of people with diabetes. The Evidation population itself also reflects a select group, representing those with the desire and ability to seek out digital health resources. Future studies should clarify the effects of digital health interventions in more diverse cohorts.
Digital interventions such as the messaging used in our study have great potential for reducing health inequities, if the barriers surrounding Internet connectivity and access to devices can be reduced.13 “We were able to engage individuals at scale with evidence-based, personalized interventions to achieve meaningful behavioral change. Overall, increasing influenza vaccination is essential to protect vulnerable individuals, including those with chronic conditions (especially with the rise of COVID-19),”said Luca Foschini, Evidation Co-founder and Chief Data Scientist.
REFERENCES
- Iuliano AD et al. Estimates of global seasonal influenza-associated respiratory mortality: a modelling study. Lancet 2018;391:1285-300. PubMed
- Putri WCWS et al. Economic burden of seasonal influenza in the United States. Vaccine 2018;36:3960-6. PubMed
- CDC. Flu Vaccination Coverage, United States, 2019–20 Influenza Season. October 1, 2020. https://www.cdc.gov/flu/fluvaxview/coverage-1920estimates.htm
- Ruiz PLD et al. Higher frequency of hospitalization but lower relative mortality for pandemic influenza in people with type 2 diabetes. J Intern Med 2020;287:78-86. PubMed
- Goeijenbier M et al. Benefits of flu vaccination for persons with diabetes mellitus: a review. Vaccine 2017;35:5095-101. PubMed
- Samson SI et al. Quantifying the impact of influenza among persons with type 2 diabetes mellitus: a new approach to determine medical and physical activity impact. J Diabetes Sci Technol 2021;15:44-52. PubMed
- Dale LP et al. Smartphone app uses loyalty point incentives and push notifications to encourage influenza vaccine uptake. Vaccine 2019;37:4594-600. PubMed
- Szilagyi PG et al. Effect of patient portal reminders sent by a health care system on influenza vaccination rates: a randomized clinical trial. JAMA Intern Med 2020;180:962-70. PubMed
- Lee W-N et al. Large-scale influenza vaccination promotion on a mobile app platform: a randomized controlled trial. Vaccine 2020;38:3508-14. PubMed
- Kindratt T et al. Health information technology use and influenza vaccine uptake among US adults. Int J Med Inform 2019;129:37-42. PubMed
- Jiménez-Garcia R et al. Influenza vaccination in people with type 2 diabetes, coverage, predictors of uptake, and perceptions. Result of the MADIABETES cohort a 7 years follow up study. Vaccine 2017;35:101-8. PubMed
- Mailchimp.com. Email Marketing Benchmarks by Industry. 2020. https://mailchimp.com/resources/email-marketing-benchmarks/
- Wood BR et al. Advancing digital health equity: a policy paper of the Infectious Diseases Society of America and the HIV Medicine Association. Clin Infect Dis 2021;72:913-9. PubMed
Read full report here




















